As a seasoned content creator and SEO expert in canine care, I know that understanding your dog's skin issues is like solving a complex mystery. 🕵️♂️ Your dog can't tell you what's wrong, and the symptoms—itching, redness, hair loss—often look frustratingly similar. But just like a skilled detective, you can learn to gather clues, examine evidence, and narrow down the suspects. This comprehensive guide will empower you to become a "skin detective" for your furry friend, learning to differentiate between the three most common culprits: fungal, bacterial, and allergic dermatitis. Remember, while this information is an invaluable tool for observation and communication, always consult your veterinarian for a definitive diagnosis and treatment plan. Your vet is the forensic lab and the chief inspector rolled into one.
🦠 The Three Suspects: A Deep Dive into Types of Canine Dermatitis
Before we can solve the case, we need to understand the potential perpetrators. Each type of dermatitis has a unique modus operandi (M.O.).
Suspect #1: Fungal Dermatitis
This suspect thrives in damp, warm environments. The most common forms are yeast (Malassezia) overgrowth and ringworm (dermatophytosis), which is actually a fungus, not a worm.
Key Clues & Evidence:
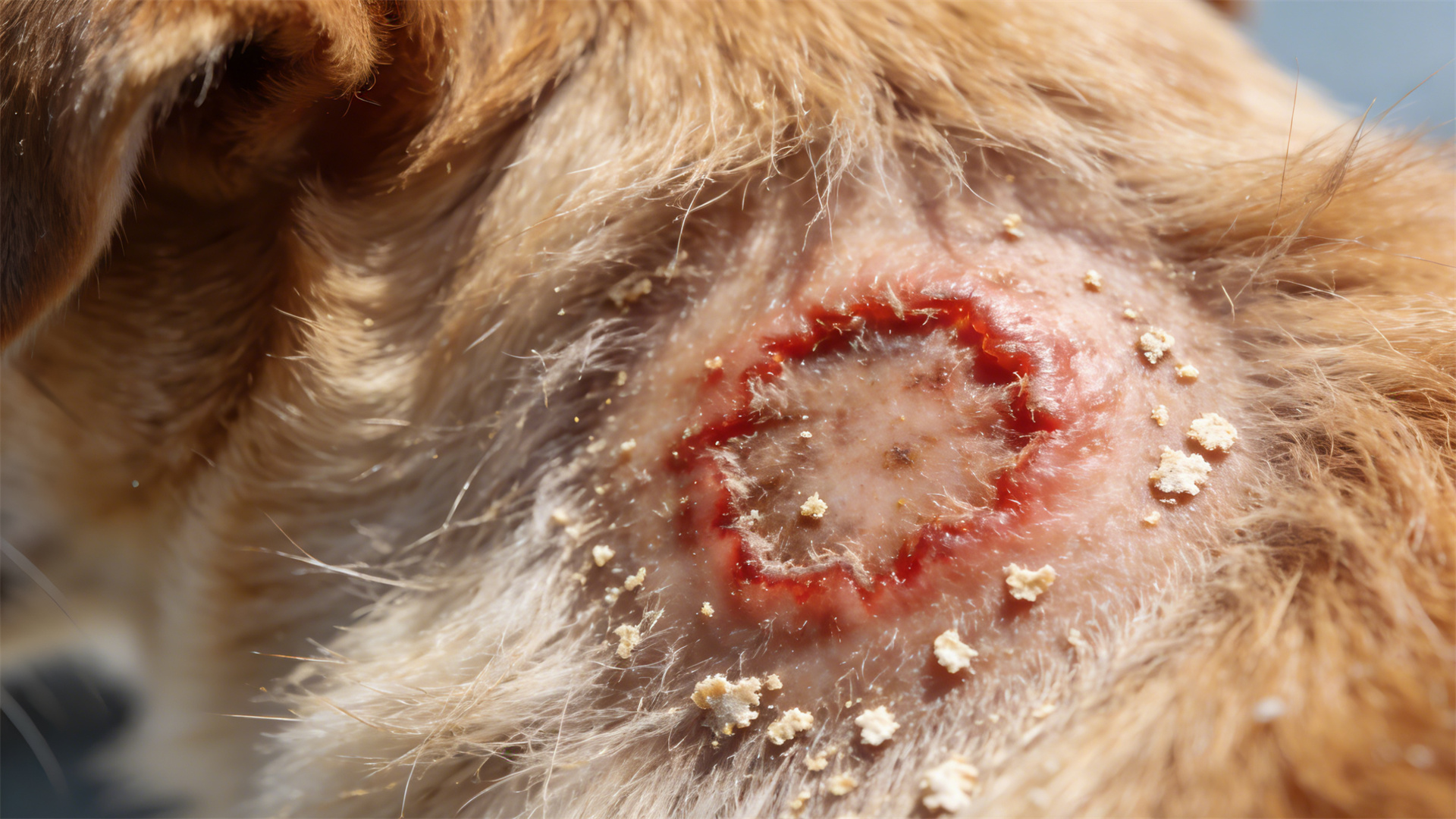
- Circular Lesions: Ringworm often presents as expanding, circular patches of hair loss with a red, crusty border, sometimes resembling a "bullseye."
- Greasy, Smelly Skin: Yeast infections love skin folds (ears, paws, neck). The skin becomes greasy, thickened, and emits a distinct, musty or cheesy odor.
- Hyperpigmentation: Chronic yeast infections cause the skin to darken (hyperpigment) and become "elephant-like" in texture.
- Contagious Nature: This is a critical clue. Ringworm is highly contagious to other pets and humans. If multiple pets or family members develop similar itchy, circular lesions, fungal is a prime suspect.
Suspect #2: Bacterial Dermatitis (Pyoderma)
"Pyoderma" literally means "pus in the skin." This suspect is often a secondary invader, taking advantage of skin already weakened by allergies, parasites, or wounds.
Key Clues & Evidence:
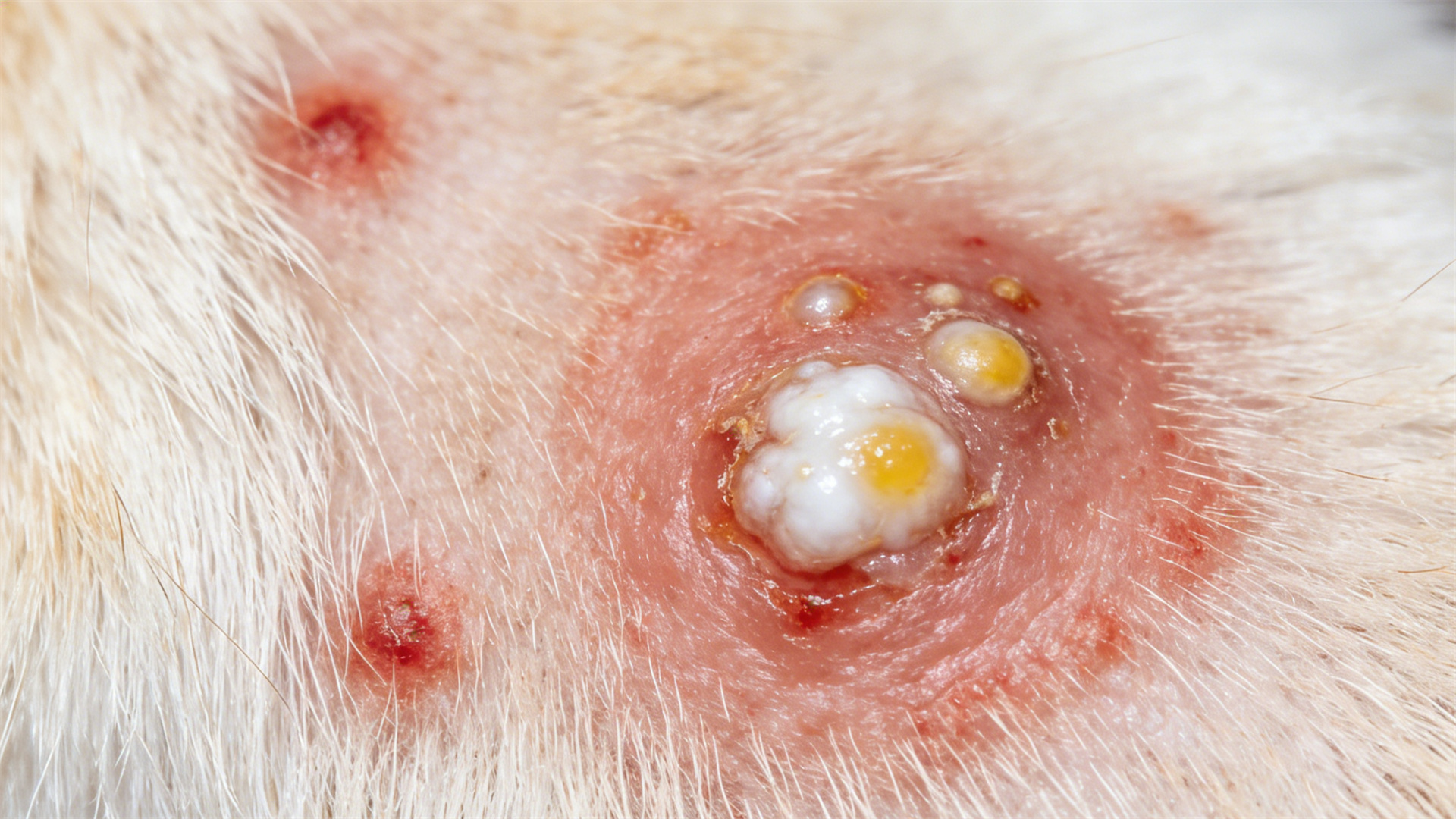
- Pustules and Papules: Look for small, red bumps (papules) or pimple-like pustules filled with pus. These are hallmarks of a surface-level bacterial infection.
- Crusts and Discharge: As pustules rupture, they leave behind yellowish crusts, scabs, and sometimes moist, weeping discharge.
- Localized or Widespread: It can appear in small, isolated spots (e.g., a "hot spot" or acute moist dermatitis) or spread over larger body areas.
- Foul Odor: The pus and infection often produce a stronger, more unpleasant odor compared to the musty smell of yeast.
Suspect #3: Allergic Dermatitis
This suspect is an internal reaction to an external or internal trigger. The immune system overreacts to allergens like pollen (atopy), food proteins, or flea saliva (Flea Allergy Dermatitis - FAD).
Key Clues & Evidence:
- Intense, Relentless Itching (Pruritus): This is the primary and most dominant symptom. Dogs will scratch, lick, chew, and rub incessantly, often targeting the paws, armpits, groin, ears, and around the eyes.
- Patterned Redness: Redness (erythema) is widespread in characteristic areas, not necessarily where the allergen touched. For example, a dog with a pollen allergy may have red paws from licking and a red belly from contact with grass.
- Recurrent Ear Infections: Chronic, waxy, and often yeast/bacterial secondary infections in the ears are a massive red flag for underlying allergies.
- Seasonal Correlation: Symptoms may flare up during specific seasons (spring/fall for pollen) or be year-round (food or indoor allergens).
🔍 The Detective's Method: A Step-by-Step Guide to Differentiation
Now, let's put on our detective hat and apply a systematic approach. This is your field guide to initial assessment before the veterinary "lab work."
Step One: Gather Initial Clues & Scene Assessment
Start with a thorough, hands-on examination of your dog in good lighting. Ask yourself:
- Lesion Shape & Pattern: Are they circular, random, or symmetrical? Symmetrical itching on both sides of the body often points to allergies.
- Location, Location, Location: Is it confined to skin folds (yeast), the back near the tail (Flea Allergy Dermatitis), or the paws/face (environmental allergies)?
- Discharge & Texture: Is the skin dry and scaly, greasy, crusty, or moist? Note any odor.
- Behavioral Timeline: When does the itching occur? After meals? After walks? Document it.
- Environmental Review: Any new food, treats, shampoo, laundry detergent, or plants? Increased flea activity?
Step Two: Examine Evidence for Contagion & Pattern
This step helps rule suspects in or out.
- The Contagion Test: Have other pets or people in the household developed similar lesions? A "Yes" strongly suggests fungal (ringworm).
- The "Secondary Infection" Pattern: Did intense itching and redness come first, followed later by pustules and crusts? This classic pattern points to a primary allergic reaction with a secondary bacterial (or yeast) infection on top.
Step Three: Analyze the Symptom Profile
Compare the core symptoms side-by-side. This is your differential diagnosis matrix.
- Fungal: Circular hair loss, greasy skin, musty smell, +/- contagion. Itching can be mild to moderate.
- Bacterial (Primary Pyoderma): Pustules, papules, crusts, pus, foul odor. Itching is variable but often present due to inflammation.
- Allergic (Primary): INTENSE itching as the #1 sign, patterned redness, recurrent ear/feet issues, often seasonal. No primary pustules—these only appear if a secondary infection develops.
Step Four: Consult the Expert – The Veterinary Forensic Lab
Your observations are crucial, but a vet provides the conclusive evidence. Be prepared to share your "detective's notebook." They may perform:
- Skin Scraping & Trichogram: Rules out parasites (mites) and can sometimes show fungal spores.
- Cytology: The gold-standard quick test. A vet takes a sample from the skin surface or pustule, stains it, and looks under a microscope. They can see yeast cells (round/oval) or bacteria (cocci/rods) in real-time, confirming a fungal or bacterial component.
- Fungal Culture: A hair sample is cultured to definitively diagnose ringworm and identify the specific species.
- Bacterial Culture & Sensitivity: For deep or stubborn infections, this identifies the exact bacteria and which antibiotics will work.
- Allergy Testing: Intradermal skin testing or serum blood tests can identify environmental allergens. Food allergies are diagnosed via a strict 8-12 week elimination diet trial with a novel or hydrolyzed protein prescription diet.

💊 Treatment and Management: The Resolution Plan
Once the culprit is identified, a targeted treatment plan can begin. Never use medications intended for one suspect on another—anti-fungals won't cure bacteria, and antibiotics won't stop an allergic reaction.
Treating Fungal Dermatitis
- Medication: Topical antifungal shampoos (miconazole, chlorhexidine), creams, sprays, or wipes. For severe or ringworm cases, oral antifungal drugs like terbinafine or itraconazole are prescribed for weeks.
- Critical Action: Environmental Decontamination. For ringworm, thorough cleaning of the home (vacuuming, washing bedding with bleach if possible, disinfecting surfaces) is essential to prevent reinfection and spread.
Treating Bacterial Dermatitis (Pyoderma)
- Medication: Topical antibiotic ointments or antimicrobial shampoos for superficial cases. Oral antibiotics are commonly needed for 3-6 weeks, and it's crucial to finish the entire course even if symptoms improve.
- Critical Action: Address the Underlying Cause. If the pyoderma is secondary, simply treating the bacteria is a temporary fix. The underlying allergy, parasite issue, or hormonal problem must be managed to prevent rapid recurrence.
Managing Allergic Dermatitis
Management, not always a cure, is the goal. It's a multi-modal approach:
- Allergen Avoidance: Rigorous flea control, using air purifiers, frequent paw washing after walks.
- Dietary Management: For food allergies, a lifelong commitment to a hypoallergenic or elimination diet is required.
- Symptomatic Relief: This may include prescription antihistamines, essential fatty acid supplements, steroids (for short-term flare-ups), or newer, targeted drugs like Apoquel (oclacitinib) or Cytopoint (lokivetmab), which specifically inhibit itch pathways.
- Long-Term Solution: Allergen-Specific Immunotherapy (ASIT) – "allergy shots" or oral drops that desensitize the immune system to specific allergens over time. This is the closest thing to a cure for atopic dermatitis.
🔚 Conclusion: Embracing Your Role as a Canine Health Advocate
Embracing the detective approach to canine skin diseases transforms you from a worried pet parent into an informed partner in your dog's healthcare. By learning to differentiate between fungal, bacterial, and allergic dermatitis, you can provide your veterinarian with high-quality observations, ask insightful questions, and better understand the prescribed treatment path. This knowledge is power—the power to reduce your dog's discomfort faster and prevent future flare-ups. Stay vigilant, stay informed, and remember: your most important case-solving tool is a strong, collaborative partnership with your veterinary professional. Your furry friend is counting on you. 🐾